Types of Phototherapy
- UVB
- PUVA
Ultraviolet light B (UVB)
UVB is present in natural sunlight and is an effective treatment for psoriasis. UVB penetrates the skin and slows the growth of affected skin cells. Treatment using UVB can include UVB phototherapy, excimer laser, or in-office or home UVB phototherapy.
UVB phototherapy treatment involves exposing the skin to an artificial UVB light source for a set length of time on a regular schedule. This treatment is administered in a health care provider’s office or clinic or at home with a phototherapy unit.
There are two types of UVB treatment:
- Broad band
- Narrow band
There are three main differences between them:
- Narrow-band UVB light bulbs release a smaller range of ultraviolet light
- Narrow-band UVB may clear psoriasis faster and produce longer remissions
- Narrow-band UVB may require fewer treatments per week
Methods of UVB Treatment
- Localized units
- Excimer laser
- Home treatment
Localized Units
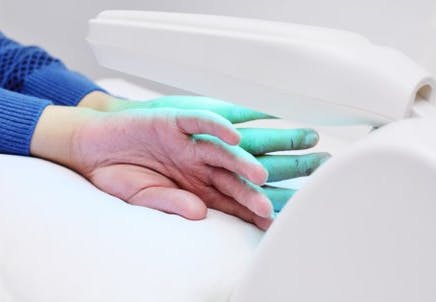
UVB treatment is offered in different ways. This can include small units for localized areas such as the hands and feet, full-body units, or hand-held units. Some UVB units use traditional UV lamps or bulbs, others use LED bulbs.
Excimer Laser
The excimer laser, approved by the Food and Drug Administration (FDA) for treating chronic, localized psoriasis plaques, emits a high-intensity beam of UVB.
The excimer laser can target areas of the skin affected by mild-to-moderate psoriasis. Research indicates it is a particularly effective treatment for scalp psoriasis. However, there is not yet enough long-term data to indicate how long improvements will last following a course of laser therapy.
Home Phototherapy Treatment
Treating psoriasis with home UVB phototherapy can be an economical and convenient choice. Like phototherapy in a health care provider’s office or clinic, it requires a consistent treatment schedule. Individuals are treated initially at a medical facility and then begin using a light unit at home. It is critical when doing phototherapy at home to follow a health care provider’s instructions and continue with regular check-ups.
All phototherapy treatments, including the purchase of equipment for home use, require a prescription from your health care provider.

%20(1).png?ixlib=gatsbyFP&auto=format%2Ccompress&fit=max&rect=36%2C0%2C550%2C316&w=778&h=447)